This profile highlights information about the health and system performance for children living in your state, district,
HRSA region or the Nation (see Methods Notes below). Part 1 presents an overview of the child population in the area you selected.
Part 2 compares your state to the Nation on a set of health status and system performance indicators. For the state selected,
indicator scores are summarized for all children, and grouped according to special health care needs and type of health insurance.
This section provides an overview of your state’s child population overall, as well as the distribution of children within each of the
two subgroups for which health and system performance measures are presented for comparison in this profile. CSHCN Status shows your state’s
estimated number and percent of children with or without special health care needs. Insurance divides the state’s child population according
to whether they have public or private sector health insurance, or currently have no insurance.
The 21 measures presented in this profile show how many children in your state have special health care needs or
chronic health conditions and how many receive health care services that meet criteria for system performance measures
related to health insurance, access to care, preventive care and medical home. For each indicator the population measured
is shown in parentheses following the description. Some measures apply to all children age 0-17; others are relevant only
for children in a smaller age range or with specific health needs and experiences.
The first two columns of the table (Overall Results) compare your state’s performance with nationwide results. The next two
columns show results for children who have special health care needs (CSHCN) compared to children without special health care
needs in your state. The last two columns compare results for children in your state who are insured by public (Medicaid, SCHIP, etc.)
versus private (individual or employment-based) health plans. Additional information about the health and quality measures is
presented in the Methods Notes below.
| CHILDREN'S HEALTH STATUS |
| Measure |
| CSHCN: Child has one or more ongoing health condition requiring above-routine amount or complexity of health services (children age 0 to 17 years) | 19.2
14,136,454 | -- | -- | 23.6
5,003,032 | 18.1
8,161,416 |
| Chronic Conditions: Child currently has one or more of 21 chronic health conditions specified (children age 0 to 17 years) | 43.0
31,728,058 | 90.2
12,755,262 | 31.8
18,972,796 | 47.4
10,060,722 | 42.3
19,066,774 |
| Weight Status: Height-to-weight ratio (BMI) at or above 85th percentile for child’s age and sex (children age 10 to 17 years) | 31.6
10,001,679 | 36.3
2,703,575 | 30.2
7,298,104 | 43.2
3,279,321 | 27.3
5,708,687 |
| Developmental Risk: Parent concerns indicate moderate or high risk for developmental or behavioral problems (children age 4 months to 5 years) | 26.4
6,135,063 | 45.4
1,277,218 | 23.7
4,857,844 | 32.7
2,621,231 | 22.1
2,936,088 |
| INSURANCE CONSISTENCY & ADEQUACY |
| Measure |
| Uninsured: Child does not currently have health insurance coverage (children age 0 to 17 years) | 9.1
6,697,766 | 6.1
858,614 | 9.8
5,839,151 | -- | -- |
| Insurance Gaps: Child is currently uninsured or was uninsured for one or more periods of time during past 12 months (children age 0 to 17 years) | 15.1
11,098,007 | 12.3
1,734,220 | 15.8
9,363,786 | 12.6
2,666,241 | 3.7
1,648,008 |
| Insurance Adequacy: Coverage does not meet child’s health needs, does not allow child to see health care providers they need, and/or family’s out-of-pocket medical expenses are unreasonable (currently insured children, age 0 to 17 years) | 23.5
15,744,885 | 29.4
3,895,577 | 22.1
11,849,308 | 18.6
3,937,768 | 25.8
11,648,633 |
| PREVENTIVE HEALTH CARE |
| Measure |
| Well Visits: Child had one or more preventive medical care visits during past 12 months (children age 0 to 17 years) | 88.5
64,575,112 | 91.4
12,802,108 | 87.8
51,773,003 | 91.4
19,056,563 | 89.5
40,129,169 |
| Dental Visits: Child had one or more preventive dental care visits during past 12 months (children age 1 to 17 years) | 78.4
54,293,506 | 84.1
11,636,399 | 76.9
42,657,107 | 76.2
14,827,895 | 82.4
35,178,486 |
| Surveillance: Parent reports that a doctor or other health care provider asked basic questions about parent’s concerns (children with health care visit in past 12 months, age 0 to 5 years) | 48.0
11,267,674 | 55.4
1,563,476 | 47.0
9,704,198 | 42.6
3,447,002 | 53.1
7,154,997 |
| Screening: Standardized developmental and behavioral screening (SDBS) was conducted during a health care visit (children who had at least one health care visit in past 12 months, age 10 months to 5 years) | 19.5
3,880,957 | 23.9
626,385 | 18.9
3,254,572 | 23.6
1,590,401 | 17.8
2,042,796 |
| HEALTH CARE SERVICE NEEDS & ACCESS |
| Measure |
| Specialist Access: Parent reports small or big problem getting specialist care for child (children who needed care from a specialist doctor during past 12 months, age 0 to 17 years) | 23.5
4,567,964 | 27.0
2,019,929 | 21.2
2,548,034 | 32.4
1,740,464 | 18.0
2,299,893 |
| Mental Health Care Access: Child did not receive mental health services in past 12 months (children who need mental health treatment or counseling, age 2 to 17 years) | 40.0
2,021,595 | 38.3
1,698,179 | 51.4
323,416 | 40.2
975,655 | 36.6
807,955 |
| MEDICAL HOME: Overall measure; Personal doctor or nurse & Usual source of care |
| Measure |
| Medical Home: Child’s health care meets all 3 basic criteria for Medical Home: (1) usual provider and place for care; (2) family-centered care; and (3) referral and coordination of health services, if needed (children age 0 to 17 years) | 57.5
40,602,320 | 49.8
6,805,059 | 59.4
33,797,261 | 45.4
9,228,041 | 66.5
28,858,804 |
| PDN: Child has personal doctor or nurse (PDN) who knows child and family well and is familiar with child’s health history (children age 0 to 17 years) | 92.2
67,685,757 | 94.7
13,352,928 | 91.6
54,332,829 | 90.8
19,179,744 | 95.4
42,875,317 |
| Usual Source of Care: Child usually goes to a specific clinic, doctor's office, or other place for medical treatment or advice when ill (children age 0 to 17 years) | 93.1
68,478,484 | 94.8
13,390,478 | 92.6
55,088,006 | 90.5
19,159,791 | 96.3
43,373,955 |
| MEDICAL HOME: Family-centered care & Care coordination |
| Measure |
| Family-Centered Care: Parent reports a trusting, collaborative, working partnership with child's health providers (children with health care visit in past 12 months, age 0 to 17 years) | 67.4
46,915,042 | 65.5
9,017,569 | 67.8
37,897,472 | 57.0
11,512,010 | 75.2
32,595,760 |
| Effective Care Coordination: Family received all care coordination wanted and is satisfied with communication among providers (children who used 2+ types of health service in past 12 months, age 0 to 17 years) | 68.7
20,570,730 | 59.3
6,055,589 | 73.6
14,515,140 | 62.7
5,874,114 | 73.8
13,615,482 |
| Care Coordination Help: Family received any help with care coordination (children who used 2 or more types of health service in past 12 months, age 0 to 17 years) | 20.7
11,141,474 | 24.8
3,149,206 | 19.4
7,992,268 | 22.9
3,521,492 | 19.9
6,881,220 |
| Extra Help Not Needed: Family did not need extra help with care coordination (children who used 2 or more types of health service in past 12 months, age 0 to 17 years) | 88.3
47,501,137 | 80.8
10,253,350 | 90.6
37,247,787 | 79.6
12,207,987 | 93.2
32,187,607 |
| MINIMAL QUALITY OF CARE INDEX |
| Measure |
| Quality Index: Child's health care meets criteria for each of three essential system performance measures: (1) adequate insurance, (2) a medical home, and (3) at least one preventive care visit in the past 12 months | 41.3
28,798,831 | 35.9
4,869,706 | 42.6
23,929,125 | 37.5
7,489,837 | 49.0
21,158,367 |
Method Notes:
1) Geographic areas: For brevity, “state” and “statewide” in this report refers to the geographical area selected, which could be any state, the District of Columbia, or a HRSA region.
2) How to read the numbers: Each cell in this profile shows the percentage of children in the group named at the top of the column
(geographic area – Nation/State, special health care needs – CSHCN/Non-CSHCN, or insurance type – Public/Private) for whom the statement
to the left at the beginning of the row (Measure or Indicator) is true. For example, the first cell in the first row shows that
“19.2 percent of children in the U.S. have special health care needs, as measured by the CSCHN Screener”.
Below the percent estimate is the 95% confidence interval (C.I.) for that estimate. The 95% C.I. is a standard widely
used among researchers to indicate a range of values that probably includes the result we would get if we were able to survey 100% of the
population represented by the sample. The difference between the upper and lower confidence limits of an estimate is a measure of the precision,
or reliability, of that estimate; narrower C.I.’s indicate more precise estimates. So another way of expressing the results shown in the first
cell for the first measure would be “The prevalence of CSHCN in the U.S. is between 18.5 and 19.8 percent of children 0-17 years of age.”
The third line in each cell shows the estimated number of children in the group described at the top of the column, for which the quality measure
statement is true: “According to the 2007 National Survey of Children’s Health, roughly 14 million children in the U.S. have special health care needs.”
3) Shaded Cells in Results Table:
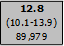 |
Percent and population estimates: Shading indicates estimate is based on sample size too small to meet standards for reliability and precision;
Relative Standard Error is 30% or more. |
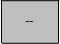 |
No results estimates shown: Shading indicates groups for which certain measures are not applicable or sufficiently reliable.
For specific information, see notes for CSHCN, Insurance Gaps, and Mental Health Care Access, below. |
4) Measures/Indicators:
Children with Special Health Care Needs: Special health care needs status is assessed by the CSHCN Screener, a standardized tool designed to identify
children with ongoing health conditions resulting in above routine health care needs. The CSHCN Screener asks whether a child currently experiences one or more of
five different health consequences: (1) uses or needs prescription medication; (2) uses or needs more than usual amount of medical care, mental health or education services;
(3) uses or needs special therapy such as occupational, physical, or speech therapy; (4) has any kind of emotional, developmental, or behavioral problem that requires
treatment or counseling; or (5) the child’s ability to do the things most other children their age can do is limited or prevented in any way. Follow-up questions
determine whether each type of health consequence is (1) the result of health condition that is has (2) lasted or is expected to last for a year or longer. Children whose
responses are “yes” to at least one item (type of special health care need) AND both follow-up question(s), qualify as having special health care needs. To learn more about
CSHCN, see our fact sheet “Who are CSHCN?” For CSHCN Screener
information - click here. Statewide results by Special
Health Care Needs are not shown because the CSHCN measure and CSHCN subgroups use the same indicator variable.
Chronic Conditions: To qualify, parent must report the child currently has one or more of the following health conditions: ADD or ADHD;
depression; anxiety problems; behavior or conduct problems; autism or other autism spectrum disorder; developmental delay; learning disability; speech problems;
Tourette Syndrome; asthma; diabetes; epilepsy or seizure disorder; hearing problems; vision problems that cannot be corrected with glasses or contact lenses; bone,
joint, or muscle problems; brain injury or concussion; hay fever or other respiratory allergy; food or digestive allergy; eczema or other skin allergy; migraine
headaches; three or more ear infections.
Weight Status: CDC guidelines for BMI-for-age are: obese - 95th percentile or higher; overweight - 85th -94th percentile; healthy weight - 5th -84th percentile;
underweight - below 5th percentile. In the NSCH, weight status is available only for children age 10 or older. For information about BMI-for-age -
click here.
Developmental Risk is assessed for children between 4 month and 5 years old, using items adapted from the Parents Evaluation of Developmental Status (PEDS).
Risk is determined from parent’s responses to age-appropriate questions about the child’s social, language, motor, and cognitive functioning. For information about how the
PEDS is used in the NSCH - click here.
Uninsured: Children who were not covered by any health insurance at the time of the survey. Statewide results by Type of Insurance are not shown because by
definition no uninsured children have insurance of any type, public or private.
Insurance Gaps: Includes children who had no health insurance at the time of the survey, or were uninsured for part or all of the previous 12 months.
Under Type of Insurance, the results shown for each group represent only currently insured children who had gaps in coverage during the past year.
Insurance Adequacy: Children’s health insurance adequate only if it meets all three of these criteria: (1) usually or always offers benefits or
covers services that meet the child’s health needs; (2) usually or always allows the child to see the health care providers they need, and (3) usually or always has
reasonable out-of-pocket expenses. A response of seldom or never to one or more of three questions indicates the child’s health insurance is not adequate.
Surveillance: Basic surveillance is met if parent reports that in the past 12 months the child had a health care visit during which a doctor, nurse or other
health care professional asked the parent if they have any concerns about the child’s learning, development, or behavior. Only children under 6 who had one or more health
care visits in the past 12 months are included in this measure.
Screening: To determine whether standardized developmental and behavioral screening (SDBS) was conducted with young children, parents were asked if they
were given a questionnaire to fill out before or during a health care visit, and if so, whether the questionnaire included age-appropriate questions about the child’s:
(1) speech and language development, and (2) behavioral and social development. Children whose parents completed a questionnaire covering both subjects are counted as
having been screened. Additional details on measurement of SDBS – click here.
Specialist Access: Pertains only to children whose parents indicated that in the past 12 months either the child saw a specialist or the parent or a doctor
thought the child needed to see a specialist. Parents were asked how much of a problem, if any, it was to get care from a specialist. Children with a response of “big problem”
or “small problem” are counted has having problems getting specialist care.
Mental Health Care Access: Counts children who did not receive treatment or counseling from a psychiatrist, psychologist, psychiatric nurse, clinical social worker, or other mental health professional during the past 12 months. This measure applies only to children age 2-17 with have any kind of emotional, developmental, or behavioral problem that requires treatment or counseling. Since this question is one of the five stem items for the CSHCN Screener, only a small number of these children were not identified by the CSHCN Screener as having special health care needs (i.e., the duration was less than one year and they did not qualify on any of the other four Screener items). For this reason, results are not shown separately in the Non-CSHCN column. However, qualifying Non-CSHCN are included in the results for other categories.
Medical Home is defined by the American Association of Pediatricians (AAP) as primary care that is accessible, continuous, comprehensive, family-centered, coordinated, compassionate, and culturally effective. The medical home measure in the 2007 NSCH is derived from 19 questions, which are used to construct several levels of component measures. This measure is a composite of indicators representing three basic medical home concepts. Part 1 is met if the child has both a PDN (personal doctor or nurse, see below) and Usual Source of Care (below). To meet Part 2 criteria, the child’s health care must qualify as Family-Centered Care (below). Part 3 includes Effective Care Coordination (below) and Referral Problems (not shown). View detailed information on Medical Home measurement in the NSCH and NS-CSHCN surveys - click here; AAP Medical Home website – click here; AAP Medical Home Policy Statement - click here.
PDN: A child’s personal doctor or nurse can be a general doctor, pediatrician, specialist doctor, nurse practitioner, or physician’s assistant; although children can have more than one personal health provider, having one PDN is sufficient to qualify for this component measure of Medical Home.
Usual Source of Care is a location the child usually goes to for care when they are sick, or if parents need advice about the child’s health. Children are not counted as having a usual source of care if their parents indicate they do not have any usual source of care or they use several places, or they usually go to a hospital emergency room or a location outside the U.S.
Family Centered Care is derived from seven validated experience-of-care questions: how often did the provider (1) spend enough time, (2) listen carefully, (3) show sensitivity to the family’s values and customs, (4) provide needed information, (5) help parents feel like partners in care, and (6) if children or parents need an interpreter, (7) provide language interpretation services when needed. Children are counted as having Family-Centered Care if their response was “Usually” or “Always” to all of the first five items and, if they needed an interpreter, the last item. Only children who saw a health care professional in the past 12 months were asked these questions. To view AAP Family-Centered Care policy statement – click here.
Effective Care Coordination: This measure applies only to children who used two or more types of health services during the past 12 months. The measure is based on two sets of questions: three items about help they needed or got with care coordination, followed by two questions about parents’ satisfaction with communication among the child’s health care providers and communication between health care providers and the child’s school or other programs. To view AAP Care Coordination Policy Statement - click here.
Care Coordination Help: Parent’s response to one of the three care coordination questions: “Does anyone help you arrange or coordinate [S.C.]’s care among the different doctors or services that [he/she] uses?”
Extra Help Not Needed: Parent’s response to one of the three care coordination questions: “During the past 12 months, have you felt that you could have used extra help arranging or coordinating [S.C.]’s care among the different health care providers or services?”
Quality Index: To qualify on this composite measure, all three of the following must be true: (1) child’s health coverage meets criteria for adequate insurance, (2) the child’s health care meets overall criteria for medical home, and (3) the child had at least one preventive care visit in the past 12 months.
With funding and direction from the Maternal and Child Health Bureau, the National Survey of Children with Special Health Care Needs was conducted by the Centers for Disease Control and Prevention’s National Center for Health Statistics. CAHMI is responsible for the analyses, interpretations, presentations and conclusions included on this site.
Suggested citation format: “[State name] Child Health and System Performance Profile from the National Survey of Children’s Health.” NSCH 2007. Child and Adolescent Health Measurement Initiative, Data Resource Center for Child and Adolescent Health website. Retrieved [mm/dd/yy] from www.childhealthdata.org.